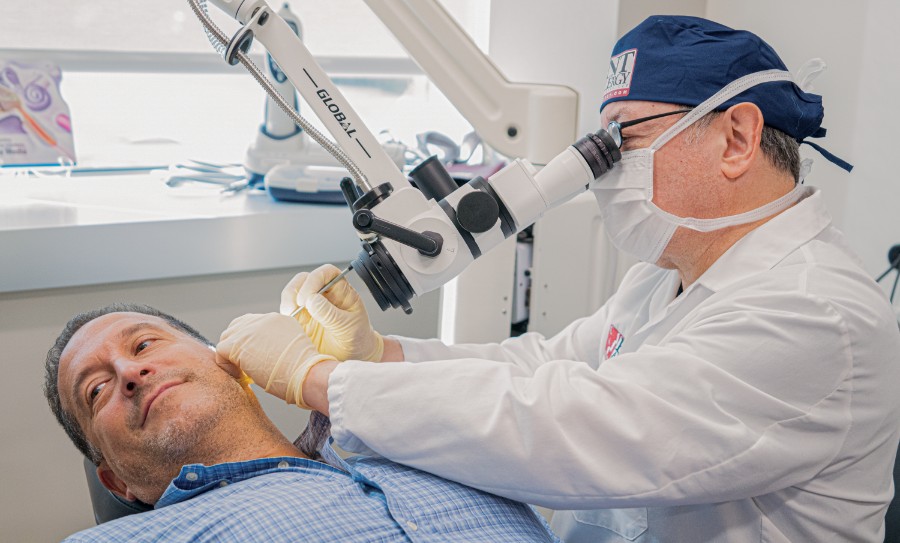
Are you or someone you know struggling with a cholesteatoma? This condition can be both painful and cause hearing loss, so it's important to find the right treatment as quickly as possible. At The Ear and Dizziness Center, we understand the challenges that come with dealing with cholesteatomas. That's why we provide comprehensive evaluations of the disease, along with customized treatment plans to ensure that your individual needs are met. Through our knowledgeable staff and evidence-based approaches, we work hard to ensure success for our patients.
What Is Cholesteatoma?
Cholesteatoma is an epithelial (skin-based) cyst originating from the tympanic membrane and is usually associated with eustachian tube dysfunction. Chronic negative pressure in the middle ear space pulls the tympanic membrane inward, creating a pocket or cyst that accumulates epithelial debris. The pocket then grows slowly and can erode surrounding structures such as the ossicles (middle ear bones), the facial nerve, the inner ear, or even the bone against the brain. The pocket also becomes a source of chronic infection, which usually does not resolve until the cyst is removed. As such, cholesteatomas can cause conductive (mechanical) and/or sensorineural (nerve-damage) hearing loss, facial paralysis, or even meningitis.
Cholesteatomas may affect all age groups, and, as a fundamentally mechanical problem, usually must be treated surgically with a procedure called a tympan mastoidectomy. A tympanostomy tube may also be inserted to address the underlying eustachian tube dysfunction.
Looking for relief from cholesteatoma or other related conditions? Look no further than our Ear and Dizziness Centers! As a subdivision of ENT & Allergy Associates, we have over 25 years of experience and a vast network of skilled physicians at our disposal. Don't suffer in silence any longer – schedule an appointment with our audiologists today and begin your journey toward optimal health and wellness.
To learn more about cholesteatoma and how we can help, contact our ear and hearing specialists today!
Patient Stories
-
"Very professional staff from the audiologist to the physician and the dr taught me something about hearing loss I was not aware of"
- Acrawl75 -
"Very personalized service from staff to Doctor especially Dr. Alaxander S."
- Shabbir A. -
"Beyond expectations, I felt comfortable, at ease, and left without any questions unanswered, knowing that his approach to my situation was working and the right course of treatment."
- R.E.
Less Sick Days, More Living

