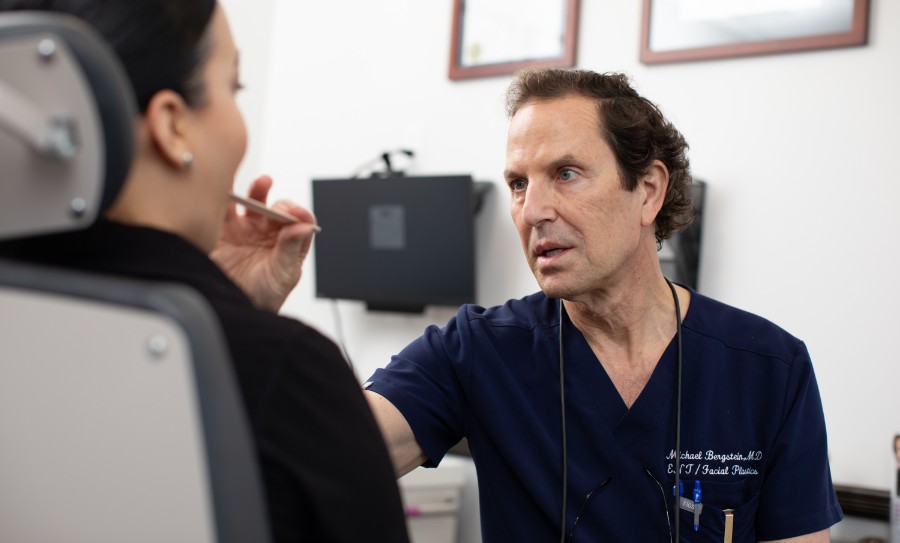
ENT & Allergy Associates, LLP is dedicated to the evaluation and treatment of voice and swallowing disorders and to further the understanding of voice and swallowing through education. The faculty at ENT & Allergy Associates has invented or pioneered a suite of office-based diagnosis & therapeutic procedures.
Swallowing Behavior Therapy
Swallowing treatment, or swallowing therapy, is divided into four broad categories: Behavioral Therapy, Dietary Therapy, Pharmacotherapy, and Surgery. The purpose of swallowing therapy is to assure a safe swallow. By safe swallow, it is meant a swallow where the chance of choking is very small. Behavioral Therapy are postural maneuvers that are implemented to ensure a safe swallow.
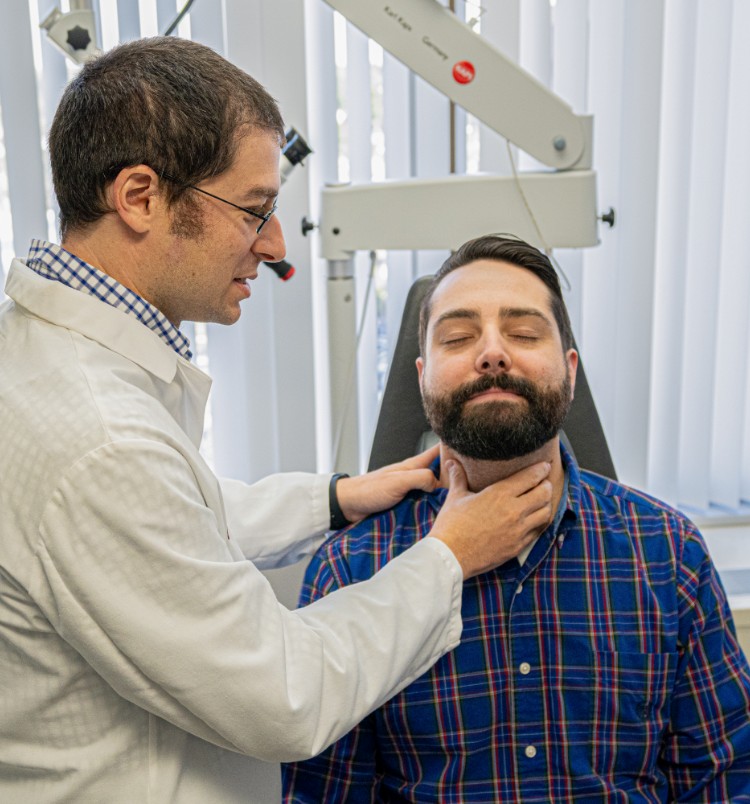
For example, a HEAD TURN is implemented when it is found that a patient is numb on one side of their throat during a FEESST exam. By having the patient turn their head to the numb side, the area of the throat that is numb becomes narrowed so that incoming food gets directed towards the sensate side of the throat.
Types of Swallowing Behavioral Therapy include:
- Head Turn
- Chin Tuck
- Effortful Swallow
- Shaker Exercises
- Supraglottic Swallow
- Mendelsohn Maneuver
Swallowing Behavior Therapy offers a sustainable and long-term solution to those experiencing swallowing problems. It provides a gentle, yet effective approach to resolving issues with proper throat muscle movement and protecting vulnerable individuals from choking and other potentially dangerous complications. Not only does Swallowing Behavior Therapy provide recovery for the patient but improves the quality of life for them as well!
Being able to swallow food or liquid normally is an integral part of daily living that many take for granted. With proper guidance from an experienced speech-language pathologist, you can finally gain control over your swallowing abilities and receive the help you need.
Contact your local office to schedule your appointment today so that you can begin your journey toward getting back what was thought to be taken away!
Patient Stories
-
"Really listens to your concerns. Super thorough & knowledgeable."
- M.L. -
"I recommend this place. Excellent staff. Fully prepared specialist. A place where you breathe peace."
- Johanna G. -
"Very personalized service from staff to Doctor especially Dr. Alaxander S."
- Shabbir A.
Less Sick Days, More Living

